Chronic Cough Workup: How GERD, Asthma, and Postnasal Drip Cause Persistent Cough
 Mar, 24 2026
Mar, 24 2026
If you’ve been coughing for more than eight weeks, you’re not alone. Around 1 in 10 adults in New Zealand and elsewhere deal with a cough that just won’t go away. It’s not just annoying-it can wreck sleep, make you tired, and even cause rib pain or urinary leaks. But here’s the good news: most chronic coughs aren’t mysterious. In fact, three common conditions-GERD, asthma, and postnasal drip (now called upper airway cough syndrome)-are behind 80 to 95% of cases in people who don’t smoke or take certain blood pressure meds.
What Exactly Is a Chronic Cough?
A chronic cough isn’t just a long cold. It’s defined as a cough lasting longer than eight weeks in adults. Unlike acute coughs from infections, chronic coughs usually don’t come with fever or mucus thickening. Instead, they’re often dry, tickly, or triggered by certain things-like lying down, eating, or breathing cold air. Many people try cough syrups, honey, or steam for months before realizing they need a different kind of help.
The key is understanding that this isn’t a single problem. It’s a signal your body is sending. Your airways are hypersensitive, and something is irritating them. The trick is finding out what.
The Big Three: GERD, Asthma, and Upper Airway Cough Syndrome
Doctors don’t start with scans or expensive tests. They start with a simple question: Could this be one of the big three?
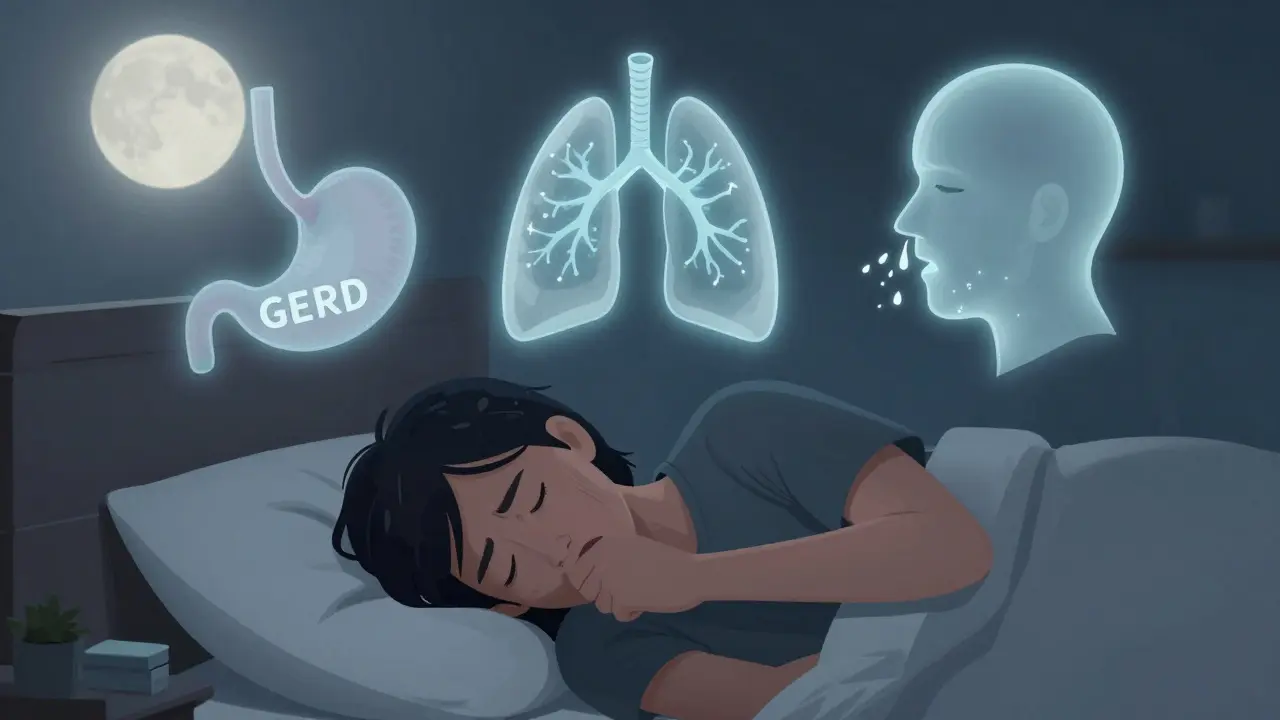
GERD (Gastroesophageal Reflux Disease) is often thought of as heartburn. But here’s the catch: up to 70% of people with GERD-related cough have no heartburn at all. This is called silent reflux. Stomach acid creeps up into the throat, irritating nerves that trigger coughing. It’s worse at night, after meals, or when lying down. Some people wake up with a sour taste or hoarse voice. Studies show only about half of these patients respond to proton pump inhibitors (PPIs), so guessing isn’t enough.
Asthma is another major player. About 1 in 4 chronic cough cases come from asthma-but not the kind with wheezing. This is cough-variant asthma, where the only symptom is a persistent cough. It often flares up during exercise, at night, or in cold air. You might not feel tightness in your chest, but your lungs are still reacting. Spirometry (a breathing test) often looks normal, which is why many people get missed. The real test? A bronchodilator or methacholine challenge. If your lung function jumps after treatment, asthma is likely the cause.
Upper Airway Cough Syndrome (UACS) is what doctors now call what used to be called postnasal drip. It’s not about mucus dripping down your throat. It’s about inflammation in your nose and sinuses triggering a cough reflex. Allergies, colds, or irritants like smoke or pollution can cause this. You might notice throat clearing, a lump-in-throat feeling, or nasal congestion. The good news? If this is the issue, you’ll usually see improvement within 1-2 weeks of using an older antihistamine like brompheniramine plus a decongestant like pseudoephedrine. Response rates are 70-90% when the diagnosis is right.
The Workup: Step-by-Step
There’s a clear path doctors follow. Skipping steps leads to wasted time and money.
- Check for red flags first. If you have weight loss, coughing up blood, fever, or swelling in your legs, you need urgent imaging. These aren’t the big three-they could be cancer, infection, or heart failure.
- Review your meds. ACE inhibitors (like lisinopril or enalapril) cause cough in 5-35% of users. If you started one within the last 6 months, switching meds might fix everything.
- Do a chest X-ray. This rules out pneumonia, lung tumors, or scarring. If it’s normal, you’re likely dealing with one of the big three. A CT scan is rarely needed unless something’s suspicious.
- Get spirometry. This breathing test checks for airflow obstruction. Normal results don’t rule out asthma-they just mean you need a deeper test like methacholine challenge.
- Try the therapeutic trials. This is where most people get stuck. Doctors don’t test for everything at once. They treat one thing at a time, with clear timelines:
- For UACS: Take a first-gen antihistamine + decongestant for 10-14 days. If your cough drops, you’ve got your answer.
- For asthma: Use an inhaler with a bronchodilator (like albuterol) for 2 weeks. If it helps, you might need a daily controller inhaler.
- For GERD: Take a high-dose PPI (like omeprazole 40mg twice daily) for 4-8 weeks. Don’t expect quick results. If you’re still coughing after 8 weeks, GERD is unlikely.
It’s frustrating, but this step-by-step method works. Trying all three at once just makes it harder to know what helped.

Why Not Just Test Everything?
You might think, “Why not do a pH monitor or a CT scan right away?” Because the data doesn’t support it.
A 2024 review in Pneumon.org found that chest CT scans in people with normal X-rays only find cancer 0.1% of the time. That’s less than 1 in 1,000. But the radiation from one CT equals 74 chest X-rays. That’s not worth it unless you have clear warning signs.
Same goes for 24-hour pH monitoring. It’s expensive, uncomfortable, and only shows reflux in 50-70% of people with suspected GERD-related cough. Many patients with normal tests still improve with PPIs-because reflux isn’t just about acid. It’s about sensitivity.
And here’s the kicker: placebo effects are strong. In clinical trials, up to 40% of people who take sugar pills for chronic cough say their cough gets better. That’s why blind trials and clear timelines matter.
What If None of This Works?
About 10-30% of people don’t respond to the big three. That’s when you dig deeper.
Other causes include:
- Chronic refractory cough (CRC): A condition where the nerves in the airways become overly sensitive, even without an obvious trigger. It’s not rare-it affects 1 in 5 chronic cough patients.
- Pertussis (whooping cough): Rare in adults, but possible if you’ve had a lingering cough after a cold. Requires a special nasal swab test.
- Chronic aspiration: Swallowing food or saliva into the lungs, often from neurological issues or weak throat muscles.
- Environmental triggers: Dust, mold, chemicals, or even air conditioning systems can keep the cough going.
For CRC, new drugs like gefapixant (approved in late 2022) and camlipixant (under FDA review as of May 2024) are showing real promise. They target the nerves that overreact, reducing cough frequency by 20% or more.
What You Can Do Right Now
You don’t need to wait for a specialist. Start here:
- Keep a cough diary: Note when it happens, what triggers it, and what helps.
- Stop smoking, avoid secondhand smoke, and cut back on alcohol and spicy foods.
- Elevate your head while sleeping-use a wedge pillow, not just extra blankets.
- Try an over-the-counter antihistamine-decongestant combo (like loratadine + pseudoephedrine) for 10 days.
- Don’t start PPIs without talking to your doctor-they can cause side effects like bone loss or gut issues if used long-term without need.
If you’ve tried all this and nothing’s changed, ask your GP for a referral to a pulmonologist. Bring your diary. Be ready to talk about your meds, your sleep, and your diet. The right diagnosis is out there-and it’s often simpler than you think.
What’s Changing in 2026?
Guidelines are evolving fast. The term “postnasal drip” is fading. Doctors now say “upper airway cough syndrome” because it’s not about mucus-it’s about nerve irritation. The Hull Cough Questionnaire is being used more often to measure how much your cough affects your life. And AI tools are starting to analyze cough sounds to tell if it’s asthma or reflux-accuracy is hitting 87% in early studies.
Most importantly, doctors are moving away from guessing. They’re using tools: validated questionnaires, simple breathing tests, and structured trials. It’s not perfect, but it’s better than years of unexplained coughing.
Can GERD cause a cough without heartburn?
Yes, absolutely. In fact, most people with GERD-related cough don’t have classic heartburn. This is called silent reflux. The acid irritates the throat and vocal cords, triggering a cough reflex without causing stomach discomfort. It’s often worse at night or after eating.
Is asthma always diagnosed with wheezing?
No. Cough-variant asthma is a real condition where the only symptom is a persistent, dry cough-often triggered by cold air, exercise, or allergens. Lung function tests may appear normal, which is why doctors use bronchodilators or methacholine challenges to confirm it. If your cough improves with an inhaler, asthma is likely.
Why do I need to try medications before testing?
Because the most common causes respond well to simple, low-risk treatments. Trying an antihistamine or PPI costs little and has minimal side effects. Specialized tests like pH monitoring or CT scans are expensive, involve radiation, or are invasive. If a simple trial works, you avoid unnecessary procedures. It’s a smarter, safer approach.
How long should I wait to see results from treatment?
It varies by cause. For upper airway cough syndrome, you should see improvement in 1-2 weeks. For asthma, it’s usually 2-4 weeks. For GERD, it can take 4-8 weeks because healing the throat takes time. Don’t stop treatment early-give it the full course before deciding if it worked.
Can I just take a PPI without a diagnosis?
Not recommended. PPIs can mask other problems and carry long-term risks like nutrient deficiencies, bone loss, and gut infections. The 2024 American College of Gastroenterology guidelines now advise against using PPIs for cough unless reflux is confirmed. Start with the least invasive option first.
What if my cough doesn’t improve after all the tests?
You might have chronic refractory cough (CRC), where the nerves in your airways are overly sensitive. New drugs like gefapixant and camlipixant are designed for this. Ask your doctor about a referral to a cough specialty clinic. There are also behavioral therapies, like speech-language pathology techniques, that help retrain the cough reflex.

Kenneth Jones
March 25, 2026 AT 03:38Mihir Patel
March 27, 2026 AT 01:38Grace Kusta Nasralla
March 28, 2026 AT 01:40Anil Arekar
March 29, 2026 AT 12:12Elaine Parra
March 29, 2026 AT 16:10Amber Gray
March 29, 2026 AT 23:42Danielle Arnold
March 31, 2026 AT 09:34Blessing Ogboso
April 1, 2026 AT 03:04florence matthews
April 1, 2026 AT 22:02