Atopic Dermatitis: Flare Triggers and Emollient Therapy Guide
 Mar, 31 2026
Mar, 31 2026
If you wake up scratching your arms or face, you know the struggle of managing sensitive skin. Atopic Dermatitis is a chronic inflammatory skin condition characterized by dry, itchy, and inflamed skin resulting from a compromised skin barrier function. Also known as eczema, this isn’t just a surface problem; it’s a deeper issue with how your skin holds moisture and defends itself. While you might see temporary relief with creams, long-term control requires understanding what sets off a flare-up and mastering the routine of barrier repair. In this guide, we break down exactly what triggers symptoms and why consistent emollient use is non-negotiable for staying comfortable.
Key Takeaways:
- Understanding the skin barrier defect helps explain why your skin reacts so easily to triggers.
- Identifying environmental and chemical irritants can prevent up to 37% of potential flare-ups.
- Emollient therapy works best when applied within three minutes of bathing to lock in hydration.
- Petrolatum and ceramide-based products offer the highest efficacy for restoring the skin barrier.
- Daily application reduces flare frequency significantly compared to on-demand use.
The Broken Brick Wall: Understanding Your Skin Barrier
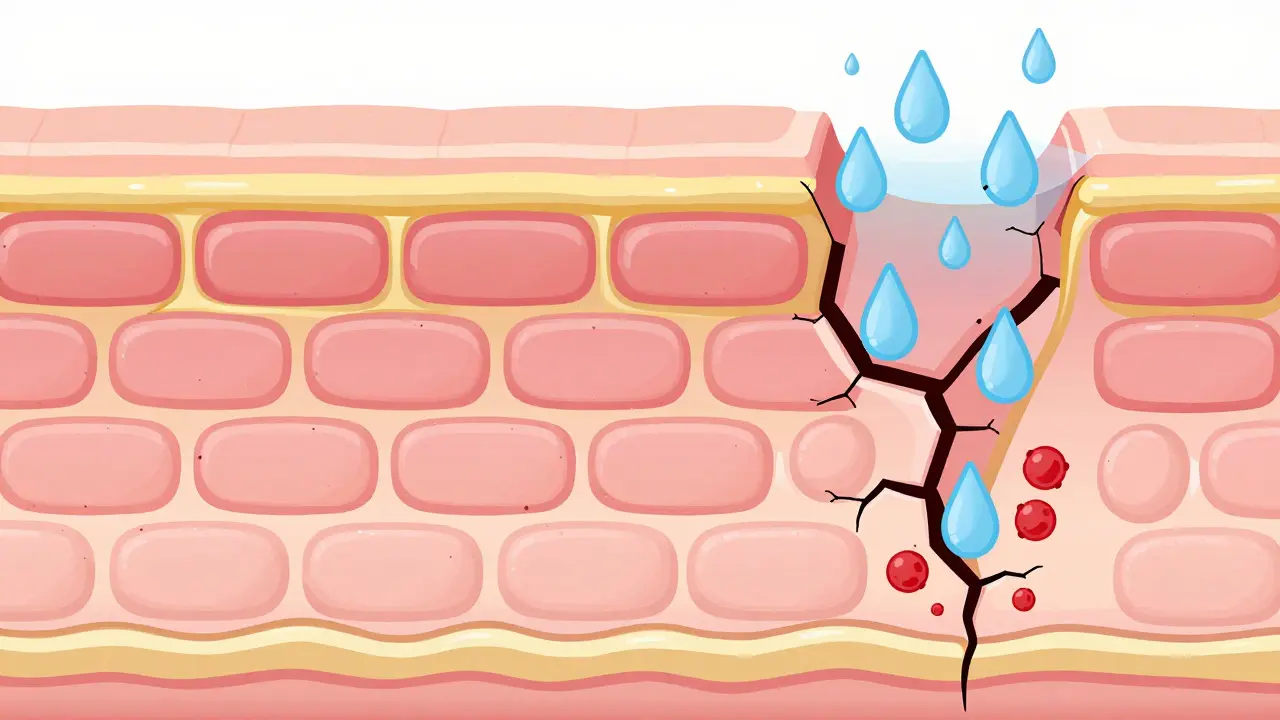
To fix the itch, you first need to understand the wall that is supposed to protect you. Think of healthy skin like a brick wall. The "bricks" are skin cells, and the "mortar" holding them together is lipids like fatty acids and cholesterol. In Atopic Dermatitis, the skin barrier is genetically impaired, often due to mutations in the filaggrin gene found in up to 50% of moderate cases. Without enough mortar, water escapes too quickly, and allergens slip in too easily.
This process is called transepidermal water loss (TEWL). In patients with active AD, this rate is measured at 15-30 grams per square meter per hour, compared to just 5-10 in healthy skin. That massive gap means your skin dries out rapidly, leading to cracks. Those cracks become entry points for bacteria like Staphylococcus aureus, which further drives inflammation and itching. Dr. Eric Simpson, a leading researcher in the field, notes that without consistent barrier repair through Emollient Therapy, no other treatment can fully take hold.
Spotting the Hidden Flare Triggers
Even with great skincare, you can’t stop every trigger. However, knowing what they look like gives you a fighting chance. Research indicates that temperature extremes play a huge role. Cold, dry air below 40% humidity increases flare risk by 37%. Conversely, heat above 80 degrees Fahrenheit triggers flares in 68% of patients because sweat contains salts and proteins that irritate broken skin.
Beyond the weather, everyday products matter immensely. Many cleansers contain sodium lauryl sulfate. Even at low concentrations of 0.5%, this surfactant strips away the lipid layer you are trying to rebuild. According to contact dermatitis studies, fragrance is another major culprit, causing reactions in 15% of patients who might otherwise tolerate a product. Before buying a new lotion or laundry detergent, check the label for alcohol, parabens, and perfumes.
| Ingredient Type | Primary Function | Efficacy Data | Best For |
|---|---|---|---|
| Petrolatum | Occlusive barrier | 98% efficacy in reducing TEWL | Severe dryness, acute flares |
| Ceramides | Lipid replacement | Restores barrier at 0.5-3% concentration | Prevention, daily maintenance |
| Glycerin | Humectant | Optimal at 40-50% concentration | Hydration retention |
| Squalane | Natural oil mimic | Well tolerated by sensitive skin | Face and delicate areas |
While natural oils sound appealing, pure plant oils sometimes lack the right balance of cholesterol and fatty acids needed to patch the "mortar" between your skin cells. Clinical trials show that formulations containing synthetic ceramides actually penetrate better than standard coconut or olive oil alone.

Mastering the Emollient Routine
You can buy the most expensive cream in the world, but if you apply it wrong, it won’t help. The golden rule taught by dermatologists is the "soak and seal" method. First, take a lukewarm bath for 15 to 20 minutes. Do not scrub hard. Immediately after stepping out, while your skin is still damp, apply your moisturizer. Dr. Amy Paller emphasizes that this timing is critical to lock in 50% more moisture. If you wait until your skin feels dry, you miss that window of opportunity.
How much should you use? Most people under-guess. The American Academy of Dermatology recommends adults use between 250 to 500 grams of product per week. That is roughly two to four tubes a month. It sounds like a lot, but think of it as food for your skin. You wouldn’t eat one meal a week, so don’t feed your skin that little either. Apply in downward strokes to avoid irritating hair follicles. Focus on areas that crack or feel tight.
When Moisturizing Isn’t Enough
Emollients are safe, but they aren’t magic cures for severe rashes. If your skin is red, hot, and oozing, the barrier damage is too advanced for cream alone. This is where topical corticosteroids (TCS) come in. They reduce the inflammation allowing the skin to heal. Studies show that combining TCS with emollients achieves clearance in 70-80% of mild cases, whereas emolients alone only reach 30-40%. The good news is emollients are safer long-term, with adverse events reported in only 2.3% of users compared to higher rates for steroids.
If over-the-counter methods fail, systemic treatments like dupilumab are becoming more available. These injectable medications target the immune pathway driving the rash. They reduce flare-ups by 70-80% in severe cases. However, even with these powerful drugs, you still need to use emollients. Think of the medication as putting out the fire and the cream as rebuilding the house.

Troubleshooting Common Hurdles
Many people quit because the product feels messy. Surveys show 30% of patients discontinue use within six months because of greasiness. If that sounds familiar, switch textures. Look for a lighter gel-cream if you live in a humid climate, or stick to heavy ointments like petroleum jelly if the air is dry. Another common pitfall is preservative sensitivity. About 5.7% of users develop contact dermatitis to preservatives like methylisothiazolinone. Always patch test a new product on a small area of your arm before covering your whole body.
Cost is also a real barrier. Prescription-grade brands average $18.99 per tube versus $8.49 for basic petroleum jelly. If budget is tight, plain white petrolatum is medically effective and widely approved by dermatology boards. Don’t stress about buying the most expensive brand with ‘medical grade’ printed on it; check the ingredient list instead. High-quality generics work just as well if the formulation is correct.
Is it okay to use emollients on baby skin?
Yes, emollients are safe for infants. In fact, applying them twice daily from birth can reduce the incidence of eczema in high-risk babies by approximately 11%, though consistency is key for any benefit.
Can I use makeup over my emollient?
You can, but choose mineral-based foundations free of fragrance. Apply your makeup over the moisturizer once it has absorbed slightly to avoid mixing textures that might clog pores or irritate the skin.
How long does it take to see results from moisturizing?
Immediate relief comes from the hydrating effect, but true barrier repair takes time. Clinical studies measure significant reduction in water loss after 2 to 4 weeks of strict twice-daily application.
Are fragrance-free options really necessary?
Absolutely. Fragrance is one of the top three identified chemical irritants for sensitive skin. Switching to fragrance-free products has been shown to eliminate flares in 15% of previously symptomatic patients.
What should I do during a bad flare-up?
During severe flares, combine thick emollients with prescription-strength anti-inflammatory medication. Wet wraps-layering damp cotton clothing over the cream-can also enhance absorption and calm intense itching.
Moving Forward with Confidence
Living with Atopic Dermatitis requires patience and discipline. The data is clear: maintaining the skin barrier prevents the itch-scratch cycle. By identifying your specific triggers like heat, humidity, or harsh chemicals, you remove half the battle. Stick to the morning and night routine, use products rich in ceramides or petrolatum, and listen to your skin’s needs rather than trends. With the right tools and habits, you can regain control and stop worrying about the next flare-up.

Divine Manna
April 1, 2026 AT 20:52The mechanism behind transepidermal water loss is frequently misunderstood by those who rely solely on anecdotal evidence.
Many individuals fail to recognize that the filaggrin gene mutation creates a fundamental structural deficit requiring more than superficial hydration.
When discussing barrier repair one must acknowledge that petrolatum functions as an occlusive agent preventing further moisture escape.
The scientific consensus regarding ceramide ratios is clear yet often ignored in favor of trendy natural oils.
Patients often mistake immediate relief for long term healing which is a dangerous distinction to blur.
We see frequent misapplication techniques where creams are applied to dry skin instead of damp surfaces.
This error negates the potential efficacy of high quality formulations by up to fifty percent.
It is essential to note that fragrance compounds introduce unnecessary variables to an already sensitive environment.
Chemical irritants found in common household cleaning agents further exacerbate the condition without warning labels.
The correlation between humidity levels and flare frequency provides concrete data for management strategies.
Temperature regulation remains another factor that requires active monitoring throughout seasonal changes.
Steroidal interventions should be viewed as temporary measures rather than permanent solutions for chronic inflammation.
Compliance with prescribed topical regimens dictates the clinical outcome more than any single pharmaceutical intervention.
Neglecting the foundational step of barrier maintenance guarantees a cycle of recurrent dermatitis regardless of potency used elsewhere.
One must accept that patience is required when attempting to restore lipid bilayer integrity.
Ultimately consistent daily application remains the most reliable predictor of symptom control.
Sam Hayes
April 3, 2026 AT 06:51that is really helpful stuff about the timing after showering I try to stick to that routine myself
feels like magic when you catch that window before the drying starts
most people think they can just slap on lotion anytime but the science backs up waiting on damp skin
i have seen friends struggle because they let their skin air dry completely before moisturizing
it takes a bit of effort but you get less itching later which is worth the trouble
i find the lighter lotions disappear too quickly in cold weather
just want to share what works for me keeping things stable
Joey Petelle
April 3, 2026 AT 14:48oh please here we go again with the medical industrial complex pushing expensive branded garbage on desperate parents
tell me they did not pay off the researchers to say ceramides work better than olive oil sitting in your pantry
i bet the big pharma guys are laughing all the way to the bank selling us this fancy nonsense
nobody wants to hear about humidity levels when the real issue is the pollution choking our cities daily
why are we obsessing over laundry detergent when the air itself is full of allergens now
it feels like a distraction tactic to keep us buying products instead of fixing the environment
trust your gut instead of some chart comparing chemical ingredients in a table
rich people get premium lotions poor people get basic petroleum jelly and both scratch anyway
Joseph Rutakangwa
April 5, 2026 AT 09:50just apply the cream while still damp and skip the scented stuff entirely
Will Baker
April 6, 2026 AT 02:36you sound like you enjoy making yourself miserable by focusing on the negatives of every situation
maybe if you stopped acting like the world is out to get your skin you would heal faster
complaining about industry greed does nothing to fix the barrier damage you suffer every morning
people actually trying to manage their health get tired of the cynicism draining the room
your attitude suggests you prefer suffering than accepting standard care protocols
stop projecting your unhappiness onto people seeking genuine help with their condition
i find this negativity quite exhausting to read through multiple paragraphs
HARSH GUSANI
April 7, 2026 AT 01:34i love this guide very much thanks for sharing😊
sometimes the doctors do not explain things clearly enough for normal people👍
using simple stuff like vaseline works best for my family💪
do not buy expensive brands they lie to you😡
stay strong and protect your skin barrier always❤️
Vicki Marinker
April 8, 2026 AT 04:44the claim regarding fragrance reactions lacks sufficient longitudinal data to support such a broad statement
while sensitivity exists the percentage cited seems optimistic given individual variance
many studies overlook genetic predisposition in favor of environmental factors alone
one must consider that placebo effects influence subjective reports of flare reduction significantly
the methodology used in these consumer trials often fails to account for concurrent medication use
relying on internet guides for medical decisions introduces risk without proper oversight
caution is advised when adopting new routines based on aggregated patient anecdotes
Sakshi Mahant
April 8, 2026 AT 06:24it is wonderful to see how different cultures approach skin care traditions alongside modern medicine
many traditional remedies align well with the principles of barrier protection discussed here
respecting personal history while learning new scientific methods helps everyone feel included in the process
we should listen to elders who managed similar conditions before advanced treatments were available
balancing ancient wisdom with current research creates a holistic path forward for families everywhere
The Charlotte Moms Blog
April 10, 2026 AT 04:57YOU MUST UNDERSTAND THE DANGERS OF PRESERVATIVES IN EVERY SINGLE PRODUCT YOU TOUCH!!!
MANY MOTHERS IGNORE THIS CRITICAL WARNING SIGN AND LET THEIR BABIES SUFFER UNNECESSARILY!!!
IT IS NOT JUST ABOUT MOISTURE IT IS ABOUT CHEMICAL EXPOSURE THAT DESTROYS IMMUNITY OVER TIME!!!
THEY PROFIT FROM YOUR PAIN WHILE YOU SCRATCH AT NIGHT DESPERATELY!!!
CHECK THE LABEL FOR METHYLISOTHIAZOLINONE BEFORE YOU APPLY ANYTHING TO YOUR BODY!!!
NEVER TRUST A FANCY BOX IF THE INGREDIENT LIST CONTAINS UNKNOWN SYNONYMS FOR ALCOHOL!!!
EDUCATE YOURSELF PROPERLY OR YOUR CHILD WILL PAY THE PRICE LATER!!!
BE VIGILANT ABOUT WHAT YOU SMELL WHEN OPENING A BOTTLE OF LOTION!!!
STOP BUYING GIFT SETS WITH FRAGRANCE ADDED FOR MARKETING PURPOSES ONLY!!!
HEALTH IS NOT A GAMBLE IT IS A CHOICE YOU MAKE EVERY DAY!!!
STAY ALERT AND READ EVERY WORD ON THE BACK PACKAGING CAREFULLY!!!
THE COST DOES NOT MATTER IF YOUR SKIN BARRIER FAILS FROM ALLERGIC REACTIONS!!!
BASIC OINTMENTS ARE SUPERIOR TO EXPENSIVE CREAMS LOADED WITH PARABENS!!!
DO NOT FALL FOR THE MARKETING BLURB PROMISING INSTANT FIXES WITHOUT SCIENCE!!!
ALWAYS PRIORITIZE SAFETY OVER BRAND NAME RECOGNITION IN SKINCARE ROUTINES!!!
Aysha Hind
April 10, 2026 AT 19:44big corporations definitely hide the truth about synthetic fragrances causing immune collapse in children today
they push these products knowing people need them but never admit the link to rising allergy rates
you should suspect any recommendation coming from a company selling the solution itself
it makes sense that natural alternatives are suppressed by the mainstream media narrative
trust independent labs over university studies funded by private grants
stay away from anything containing hidden alcohol derivatives masked as preservatives
Lawrence Rimmer
April 11, 2026 AT 06:01suffering is merely the absence of understanding your own body signals in a complex universe
we chase cures while ignoring the deeper disconnect between modern living and human physiology
perhaps the itch tells us something about stress rather than just dryness alone
medicine treats the symptom while philosophy asks why the symptom appeared initially
true wellness requires looking beyond the jar of cream and examining lifestyle choices fundamentally
Hudson Nascimento Santos
April 11, 2026 AT 11:16the nature of inflammation reflects an internal conflict within the organism seeking homeostasis against external chaos
treating the surface ignores the systemic harmony disrupted by the trigger event
one must contemplate whether the cure lies in suppression or restoration of balance
wisdom comes from recognizing the barrier as a boundary between self and environment
managing this requires patience and reflection on daily habits more than medication
Dipankar Das
April 12, 2026 AT 06:06Your dedication to managing this condition demonstrates significant resilience and commitment to long term health outcomes
Consistent adherence to emollient therapy establishes a foundation for improved quality of life over time
Patience remains the most valuable asset when navigating the fluctuations inherent to chronic skin conditions
Please remember that progress is often measured in weeks rather than days during active recovery phases
Maintaining a positive mindset supports the physiological healing process effectively
Joey Petelle
April 13, 2026 AT 18:32lol this thread went philosophical fast and now back to basics